Conditional cash transfer (CCT) programs are now widespread in Latin America. Fifteen countries run CCT programs, benefiting approximately 100 million people and 21 million households.
These programs address market failures associated with low investment in human capital for the poor. Although their structure differs by country, CCTs generally transfer cash to poor mothers once they have accessed certain public programs such as preventive health services and ensured school attendance for their children. The programs also provide counseling and education on better health and nutritional practices. In effect, CCTs combine short-term transfers for income support with incentives for long-term investments in human capital.
By transferring resources directly to poor households—generally 10 percent to 30 percent of a household’s average monthly spending—CCTs intervene on the demand side to change relationships between health service users, service providers and governments. They do not directly intervene on the supply side; but they indirectly address market failures, such as disincentives for coordination and information asymmetries by producing detailed information on gaps in the supply of health and education services to marginalized populations.
Accountability
By increasing demand and revealing gaps in quality and availability, these programs indirectly generate political pressure to improve public services.
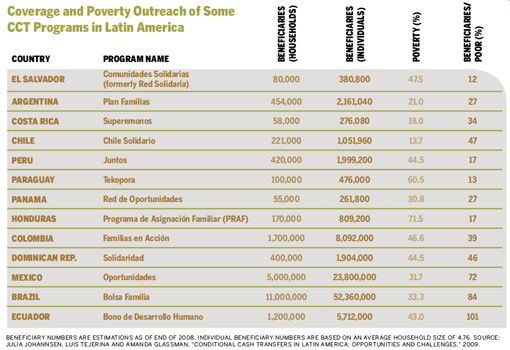
Overall, CCT programs are extremely progressive. The majority of benefits do reach the poor [see table]. There is some leakage to wealthier groups, but this is a problem for any kind of income proxy means test.
Looking specifically at health care, without any intervention, the use of public health services by the poor is low and health outcomes are highly unequal between the poor and the rich. In Nicaragua, for example, 2006–2007 survey data indicate that stunted growth affects only 6.1 percent of children nationally, but 11 percent of children from the country’s poorest quintile.1 Likewise, in Honduras, 2005 data show that stunting is high at 25 percent of children nationally and a shocking 43 percent for children in the poverty income bracket.2
The development implications of these health inequalities are substantial. Improved nutrition in early childhood leads to better adult human capital including larger body size, improved physical work capacity, better cognitive skills, and higher earnings.
These large inequalities between rich and poor in health outcomes and the use of health programs are partly what drive CCT programs.
CCTs expand the use of preventive services by the poor. This includes increases in public health visits and immunization rates across Latin American programs. But the evidence is mixed on health and nutrition outcomes. CCT programs in Mexico, Nicaragua and Colombia have a positive impact on the prevalence of stunting among young children. However, programs in Honduras and Brazil show no noteworthy effects.
Results for the proportion of underweight children are less consistent. Nicaragua’s program shows a significant decline, while the Honduras program finds no impact. In Colombia, the benefits of CCTs on nourishment are only seen among three to seven year-olds in rural areas. Whereas in Mexico, a positive effect of the CCT program on the weight of children up to six months old is found only in urban areas. Here, too, CCT participation implied a 44.5 percent reduction in low birth weight in rural areas.
Satisfaction
Overall, the poorest families perceive the most benefit from CCTs. The CCT program in Mexico was responsible for improved height-for-age in the children of beneficiary women with no formal education. Meanwhile, there are similar findings regarding vaccination rates in rural areas of Mexico, Honduras and Nicaragua that benefit from transfer programs.3 Even beyond the health and nutrition impact, Latin American CCT programs positively affect school attendance and progression and poverty rates.
CCTs may not be the perfect answer, but their positive effects suggest that restricting the programs to the very poorest can be a fruitful strategy to improve impact. While CCTs continue to face design and implementation challenges, particularly related to the quality of the supply-side services, the multidimensionality of CCT programs (consumption, health, nutrition, education) and their targeting of poverty represent powerful levers to improve the well-being of the poor.
Footnotes
1. Based on IDB staff calculations of Encuesta Nacional de Demografía y Salud, 2006-2007.
2. Ibid.
3. Barham and Maluccio (2009) review some of the studies on CCTs and vaccination rates. In Mexican rural areas, they find small average effects of the CCT program Oportunidades, on the order of 3 percentage points, and argue that this is due to high coverage rates (above 90 percent) before the program. In rural Honduras, a conditional voucher program yields significant increases for the first dose of the DPT vaccine and no effect for the meningococcal conjugate vaccine (MCV). In Nicaragua, the Red de Protección Social (RPS) CCT, which began in 2000, led to large increases in vaccination coverage with the effects particularly large for those sub-populations that are traditionally harder to reach including children who live further away from a health facility or whose mothers are less educated.